Supporting Pharmacy for Indigenous and Rural Australians
Software and Services
to Support Pharmacies in Rural and Remote Areas



Software and Services
to Support Pharmacies in Rural and Remote Areas

How do you provide medication counselling, information and support to patients that rarely (or never) walk into a pharmacy?

How do you safely manage medications for patients who are continually transitioning between primary care clinics, hospitals, renal centres and aged care facilities?

How can you make health services feel that community pharmacists working for a separate organisation feel like part of their team?

How can pharmacists help other health practitioners focus more on their clinical specialties by taking on a greater share of medication-related work?

How can pharmacy owners make sure that patients, health practitioners and clinic staff always receive the same high level of service irrespective of which pharmacy or pharmacist they're engaging with?

How can pharmacies and clinics onboard staff quickly so that patient safety is maintained even with staff turnover and a locum-heavy workforce?

How can we make sure that pharmacies communicate effectively with all stakeholders without pharmacists spending all day talking on the phone or emailing?

How can all of the above be achieved in a financially sustainable way so that the pharmacy can support the community indefinitely?

How can pharmacies better track the work they do so they can demonstrate the value of pharmacy services to the policy makers who make decisions on service delivery and funding?
Rural/remote pharmacies operate very differently from city-based pharmacies. Like all pharmacies, they dispense scripts, managed controlled drugs, pack DAAs and provide clinical services. But in rural/remote areas, where there is usually only one pharmacy in a given town, the pharmacy is a "shared resource" for the whole healthcare sector. These pharmacies are not only providing services to patients, but they provide services to hospitals, town-based and remote clinics, renal centres and aged care facilities.
because there are so few rural/remote pharmacies, software tailored to their specific needs does not exist
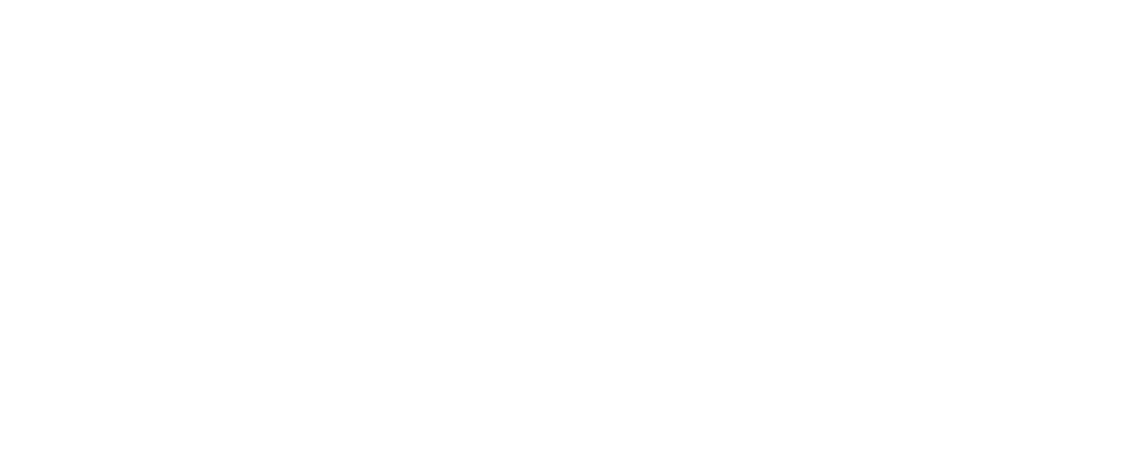
All pharmacies dispense scripts, manage controlled drugs, provide clinical services and many pack dose administration aids (DAAs). There are established vendors that provide software to cover these four areas.
However, rural/remote pharmacies do work that is not typical for city-based pharmacies such as:
Moreover, in order to provide those front-line services, a lot of work happens behind the scenes. This includes such things as:
But the solution is not more software.
Adding more software just creates a different set of problems. What is needed is software that allows rural/remote pharmacies to do everything they need to do - all in one place. That means:
Care that is safe across all practice settings is critical. Spira has been built not only to ensure the safe and accurate supply of medicines, but to support pharmacy staff and clinicians to provide care that is culturally appropriate, safe and accessible for all patients, families, communities and clinicians.
Spira aims to close gaps in medication understanding and access for the betterment of health for all.
Spira has strong relationships with our Kimberley ACCHOs to provide solutions tailored to technical and cultural needs. This includes things like customised labelling of medicines, language and communication platforms to support medication and health literacy.
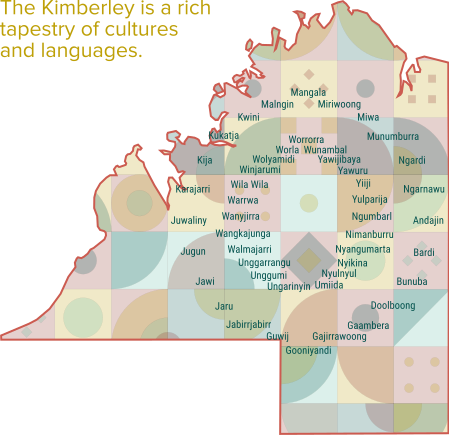
City-based pharmacies have a direct relationship patients because their patients walk into the pharmacy. In rural/remote areas, a large number of patients will never walk into a pharmacy. Pharmacy services are provided to patients through clinics and other clinicians.
Providing pharmacy services to patients that may never be seen in a pharmacy requires a specific type of software.
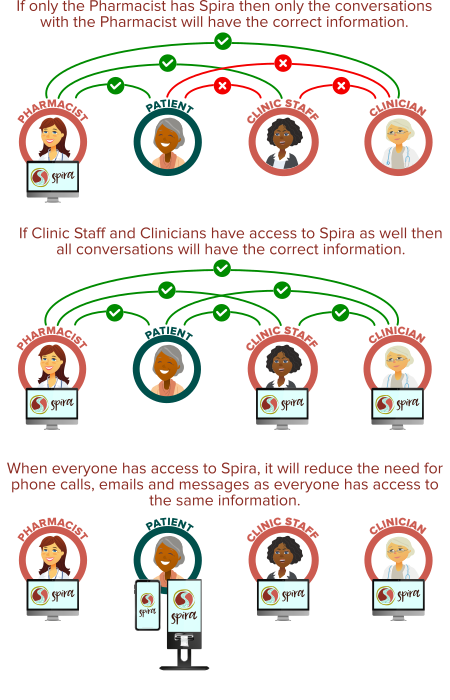
The same message must get through to the patient, no matter how many people are between the pharmacist and the patient. Patient trust is undermined if they're not hearing the same message from everyone they're engaging with (Pharmacist, Clinicians, Clinic Staff).

When a Pharmacist talks to a patient, the Pharmacist must know:

When a Pharmacist talks to a Clinician, the Pharmacist must know:

When a Pharmacist talks to Clinic Staff, the Pharmacist must know:

Every pharmacy wants to provide a "good service". But in order to build software, we need to have a clear definition of "good service"".
Good intentions and good people are important, but in order to truly deliver a good service you need technology.
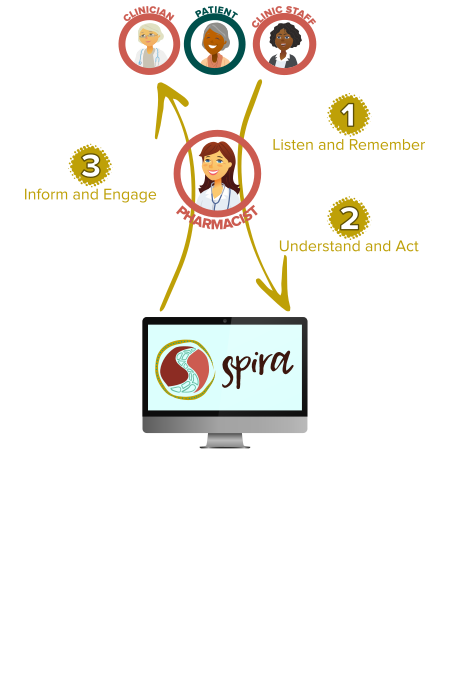
Spira defines "good service" as the ability to listen and remember, understand and act and finally engage and inform. All of these things need to be done consistently well.

Patients, Clinics and Clinicians tell us things.
People are better at listening, but software is better at remembering. Pharmacists can listen to and connect with Patients, Clinicians and Clinic Staff, but the information collected needs to be stored somewhere. It's not "good service" if stakeholders have to say the same things over and over again to different people.

Patients, Clinics and Clinicians request things.
People are better at understanding what needs to be done, but software must make it easy to do. Pharmacists can have discussions with Patients, Clinicians and Clinic Staff to clearly understand what needs to happen. Once everyone understands and agrees what has to be done, it actually has to be done. It's not "good service" if requests are forgotten or not fully actioned.

Patients, Clinics and Clinicians ask for things.
Pharmacists need to be able to answer whatever questions they're asked. Eventually, the pharmacy can go from reactively answering questions, to proactively engaging with Patients, Clinicians and Clinic Staff by answering questions before they're even asked. It's not "good service" if you can't answer the questions your stakeholders are asking, or if you can't anticipate their needs.
Productivity experts call it 'One Touch'. Customer service experts call it 'First Contact Resolution'. Software experts call it 'Single Pane of Glass'. Whatever you call it, the principle is simple: have all of the information and functionality in front of you so you can do what you need to do, the first time you do it.
Every time an enquiry, request or task is parked or handed over, you're introducing inefficiencies, creating work, and adding risk that something falls through the cracks.
Spira is built so there are no handovers and there's no 'parking' something and coming back to it later. It allows staff to fully complete a task, fully answer an enquiry, or fully action a request so the work is fully "done done". No scrap pieces of paper, no Post-It notes, no emails-to-self, no 'I will have to get back to you', no coming back to it later.

Spira allows conversations (or emails) to be fully documented so everyone in the pharmacy knows what has been said by Patients, Clinicians and Clinic Staff.

Spira allows requests to be fully actioned so everyone in the pharmacy knows what has been requested by Patients, Clinicians and Clinic Staff.

Spira allows enquiries to be fully answered the first time, and ensures that Patients, Clinicians and Clinic Staff get the same answer.

It's no secret that rural/remote pharmacies have workforce challenges. Even if a pharmacy could attract all the pharmacists it wanted, it would not be financially viable to do so. Pharmacists in rural/remote areas not only get paid significantly higher salaries, but they typically have additional annual leave, receive free accommodation, have their bills paid and have a range of additional perks. Put simply, pharmacists in rural/remote areas cost more.
There are also challenges around recruiting and retaining support staff. Rural/remote pharmacies are competing with Government departments and mining companies for qualified staff, which means pharmacies might have to take a chance on less experienced or less qualified staff. Such staff tend to require additional oversight and supervision, further adding to pharmacist workload.
Software has a key role to play in reducing workforce challenges by making existing staff as efficient as possible.
There's a number of things that software can do to increase workforce efficiency. The bonus is that increasing efficiency makes everyone's lives easier, leading to improved job satisfaction and staff retention.

A lot of time and effort goes into tracking things. Has that been done? Did we get that script? Where are we at with X? Did that doctor get back to us? Pharmacists are walking around with an ever-growing 'To-Do' list in their heads.
Software can keep track of what needs to be done, monitor progress and notify pharmacists of potential issues before they become problems.

Pharmacists are ultimately responsible for what happens in a pharmacy so they want to be sure that support staff have the skills necessary to perform a task before the pharmacist feels comfortable delegating it. Pharmacists are busy enough being pharmacists and shouldn't be doing work that can be done by non-pharmacists.
Software allows support staff to perform tasks with appropriate guard-rails so pharmacists can delegate tasks with confidence.

Delegation is not abdication. If a pharmacist delegates a task to someone, they are still accountable for making sure it gets done. But keeping track of everything is hard and sometimes pharmacists find it easier to just do the work themselves.
Software can keep track of who is supposed to do what and by when, and can alert pharmacists if things get off track.

Not all the work that needs to be done in a pharmacy needs to be done by a person. Running reports, billing/invoicing, sending reports/extracts/notifications to clinics and monitoring data (e.g. script expiries, stock levels) are things that should not need human intervention.
Software makes sure that anything that can be done by a machine, is done by a machine.

A lot of effort is wasted in pharmacies chasing information in various systems that don't talk to each other. Worse still, a lot of information needs to be double-entered into multiple systems. If information is in more than one place time is wasted figuring out which system has the most up-to-date version of that information.
Software makes sure that staff have everything they need to do their work in one place.

Pharmacies receive quick and routine enquiries and requests all the time. And often it's the same enquiries/requests over and over again. Minimising the time and effort it takes to handle these, frees up a lot of time.
Software can make repetitive tasks quick and easy to do.
These days everyone expects some level of self-service - we bank online, we plan our own travel and we order food without calling a phone number. Allowing stakeholders to do things for themselves not only makes their life easier, it reduces the workload on the pharmacy.
Software allows external stakeholders to do everything that the pharmacy can do, and see everything that the pharmacy can see.
Just giving stakeholders access is not enough. They don't have the time to learn yet another system. Everyone should have easy access to the information and functionality they need without having to hunt for it.

The overwhelming majority of emails, phone calls and messages coming into a pharmacy are simple transactions. A Patient, Clinician or Clinic Staff just want to know something or request something very simple. It often takes less time to answer the question or fulfil the request than it takes to write the email/message of make the phone call. These enquiries/requests are ideal for self-service.

When one person is reading the information on their computer screen to someone else over the phone, there's a chance that the information is misinterpreted. This is especially risky if it's a clinical conversation. And even in written responses aren't ideal because they tend to omit context. It is much safer if everyone can see the same information for themselves.

Trust is built when everyone has access to the same information and is saying the same things, and eroded when different people are saying different things. This is true for all stakeholders, but particularly important for Patients. Pharmacists, Clinicians and Clinic Staff must be on the same page when communicating with Patients.
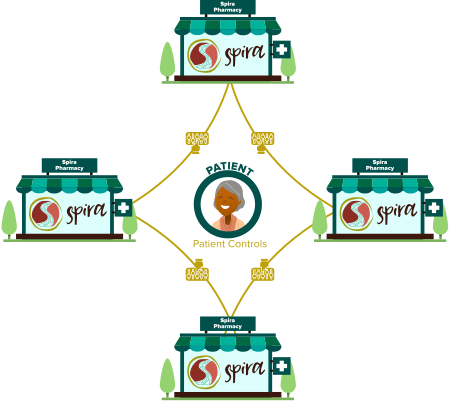
Patients have a right to privacy and respecting their wishes is fundamental to building trust between the patient and the pharmacy.
Information sharing should be subject to privacy controls.
Spira is built from the ground up to support information sharing and includes robust privacy controls to allow patients decide what information is shared and with whom.
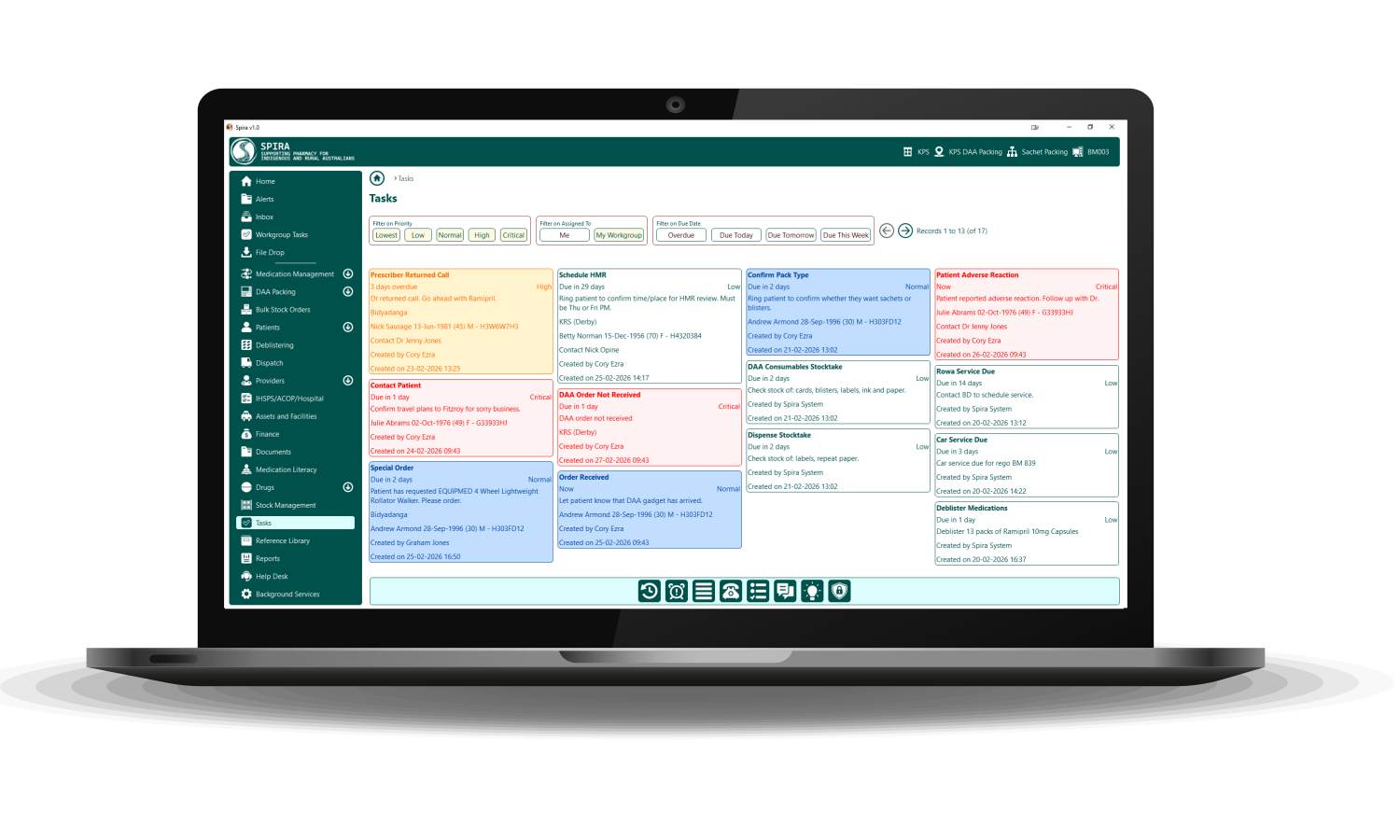
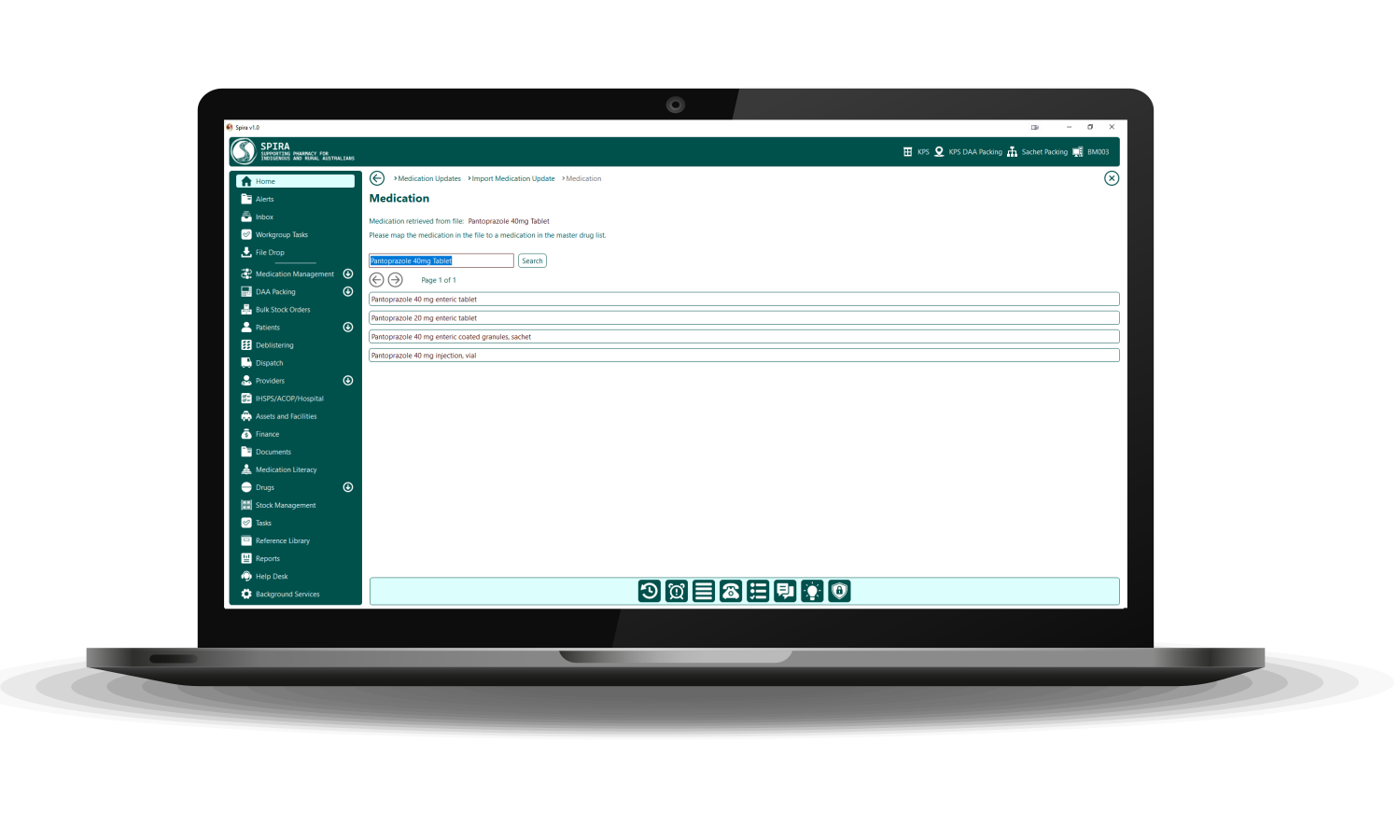

In-clinic and remote support across the funded areas of pharmacist support, patient and clinic staff education, medication reviews and policies for medication prescribing, supply, storage and management.

Health Service accreditation support in areas of medication management for RACGP, National Safety and Quality Primary and Community Healthcare Standards and the Strengthening Aged Care standards

Working with the clinical team to deliver robust and effective policies to support safe practice across all organisational roles. These policies include cold chain, monitored medicines, medication prescribing, storage, supply and administration, antimicrobial stewardship and medication safety.

Work with clinicians to design and deliver tailored auditing and monitoring reports for all areas of medication prescribing and supply.

Support in the delivery of high quality patient centred medication management solutions that are culturally appropriate and co-designed with communities.

Oversee S100 RAAHS claiming and audits to ensure accurate claiming is done in an efficient and auditable manner.

Medication reviews or Aged Care onsite pharmacist models of support including clinical reviews, staff training, resident education, imprest management, clinical governance and auditing.

Deliver face to face or online medication training to clinic staff with a focus on Aboriginal Health Workers, Practitioners, Aged Care support and Medication Officers.

In-hospital support for medication reconciliation, discharge planning, clinical support and patient education.
Kimberley Pharmacy Services (KPS) is based in Broome and provides pharmacy services to patients and clinics across the vast Kimberley region of Western Australia. As the number of clinics and patients grew, so did the number of pharmacists. It was becoming increasingly difficult to provide a consistently high level of service across the region. While rigorous onboarding and ongoing training is important, it became evident that manual procedures and ever-growing policy/procedure manuals weren't going to cut it. A technology solution was needed.
The technology solution is Spira (pronounced 'spy-ra'). Out of all the pharmacies in Australia, only a small fraction do what KPS does. With such a small market, no commercial products exist, so KPS made the decision to build the software from scratch. Spira is built for ALL rural/remote pharmacies and is currently being used by non-KPS pharmacies inside and outside the Kimberley. With Spira, patients and clinics receive the same consistently high level of service from every pharmacy and pharmacist they engage with.
the software is built in collaboration with pharmacies and pharmacists
who need to get real work done in the real world, with real patients and real clinics


Email: hello@spira.au